European Antibiotic Awareness Day 2015

Today is Antibiotics Awareness Day! This annual European public health initiative takes place on the November 18th to raise awareness about the threat to public health of antibiotic resistance and the importance of prudent antibiotic use.[1]
The Problem
Hundreds of different active antimicrobial compounds are being discovered in the environment all over the world. Concern is increasing about the harm these might be doing to human health and the environment.
How are Antibiotics harmful to the environment?
The active ingredients in antibiotics are designed to stimulate a response in humans and animals at low concentrations. Moreover, antibiotic substances are often engineered so that they remain unchanged during their passage through the body. Unfortunately, this stability means that they also persist outside the body and, as a consequence, can build up in the environment. Although levels are usually too low to result in acute effects such as organ damage, there are many cases globally where drugs have had drastic effects on the environment. For example, there is evidence that antibiotic resistance in soil can disturb ecological functions, affect the diversity of soil micro-organisms and carry out a negative impact on beneficial mycorrhiza (a type of fungus). In aquatic eco-systems, antibiotics have shown to reduce the growth of primary producers like plants and algae and have also been detected in fish.[2]
AMR
The misuse of antibiotics and their release into the environment is also contributing to the growing problem of Anti-Microbial Resistance (AMR). The more antibiotics that are used, the less effective they become as resistant bacteria develop to counteract their effects. This gives rise to AMR, caused by these resistant bacteria. According to the World Health Organization, AMR is responsible for 25,000 deaths a year across the EU and already has an economic burden of 1.5 billion euro.[3]
Solutions Along the Life Cycle
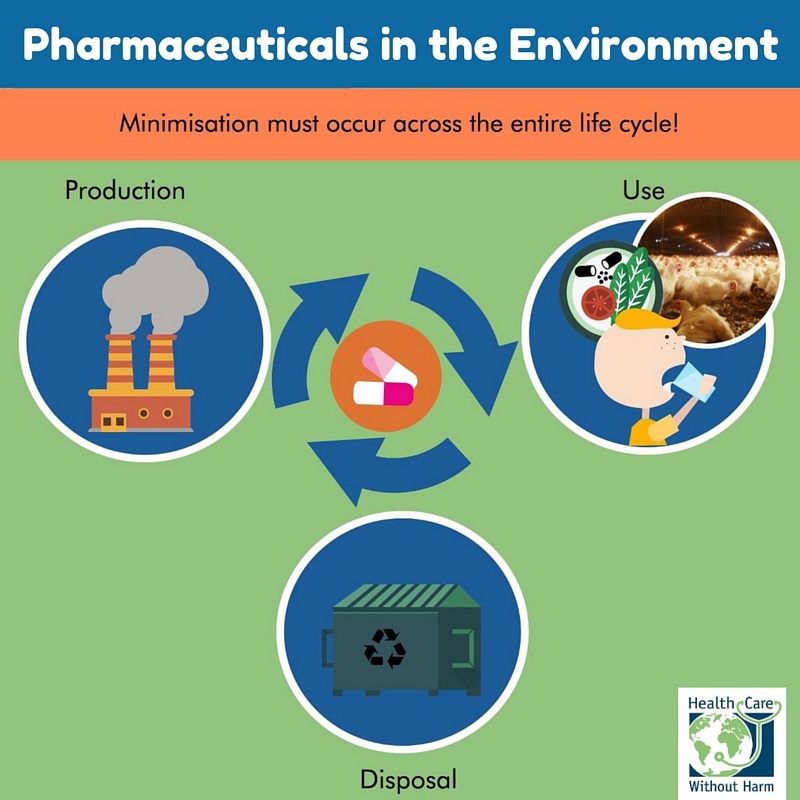
The active ingredients in antibiotics are needed to tackle harmful bacteria in humans and animals, and it is therefore very difficult to change their make-up. The minimisation of the release of antibiotics into the environment must take place along each of the stages of the drug’s life cycle. Action must be taken to minimise the use and release of antibiotics during their production, use, and disposal.
Some of our Recommendations
Production
- Manufacturers must follow environmental regulations, and should be held accountable for the products they place on the market.
- Factories must also implement prevention and mitigation systems for spills and the release of harmful substances.
- Companies and suppliers need to be more stringent with environmental permits such as licenses, registrations and restrictions.
- Companies need to know their supply chains in order to make environmentally sound business decisions.
- Policies that demand greater transparency throughout the supply chain are necessary.
Use
- In order to reduce the excessive consumption and disposal of antibiotics, health institutions and professions should improve prescription practices and promote healthy lifestyle choices.
- Health institutions and professionals should become leaders in educating patients about the harmful impacts of pharmaceuticals on the environment.
- All health institutions should provide collection services for citizens to dispose of their antibiotics safely.
- Patients must also take responsibility in their own practices, by following a healthy lifestyle and finishing their prescriptions
- When using antibiotics for food production: farmers should minimize the use of antibiotics in agriculture, and regulate contaminants in fertilizers.
Disposal
- Health institutions should implement appropriate urine collection services for specific patient groups for separate treatment, and should also implement advanced water treatment systems.
- Patients should dispose of excess medication safely.
- Food producers must also take responsibility for safe disposal of antibiotics, and make sure that contaminated waste is not released into rivers or soil.
Take a look at our infographic illustrating our recommendations for the minimization of pharmaceuticals in the environment at all stages of their life cycle.
Our Work
Raising awareness about the health and environmental issues relating to the misuse of antibiotics and pharmaceuticals is a key focus of our work at Health Care Without Harm Europe. We recently attended the fourth session of the International Conference on Chemicals Management (ICCM4) for the Strategic Approach to International Chemicals Management (SAICM) in Geneva, where we worked to encourage countries and agencies to take part in the global efforts to reduce pharmaceutical pollution in the environment.
Check out this blog post to find out more about our work at SAICM
HCWH Europe published a report, “Unused Pharmaceuticals Where Do They End Up?” which outlines the results from a survey carried out in six European countries to understand the general public’s approach to disposal of unwanted medicines and to help assess the efficiency of existing pharmaceutical collection schemes in these countries. We also published a guide for doctors, providing advice on simple practices to help reduce unnecessary pharmaceutical emissions from entering the environment.
The environmental and health risks associated with the over-prescription of antibiotics, pollution from pharmaceutical production, and the improper disposal of unused antibiotics cannot be ignored. Spread the word about the potential harms of antibiotics in the environment, and make sure you adopt these recommendations in your own practices.